 At our first critical care congress in the late '70s, there was an extraordinary amount of interest, and so we began to pursue that. So we started looking at the role of using physiology of a patient in the intensive care unit and to then develop a comprehensive measure of severity that could at least begin to discriminate one patient from another better than the DRG. But that only applied to head trauma patients and emergencies. Then Bryan Jennett created the Glasgow Coma Scale score, and was very successful with that. 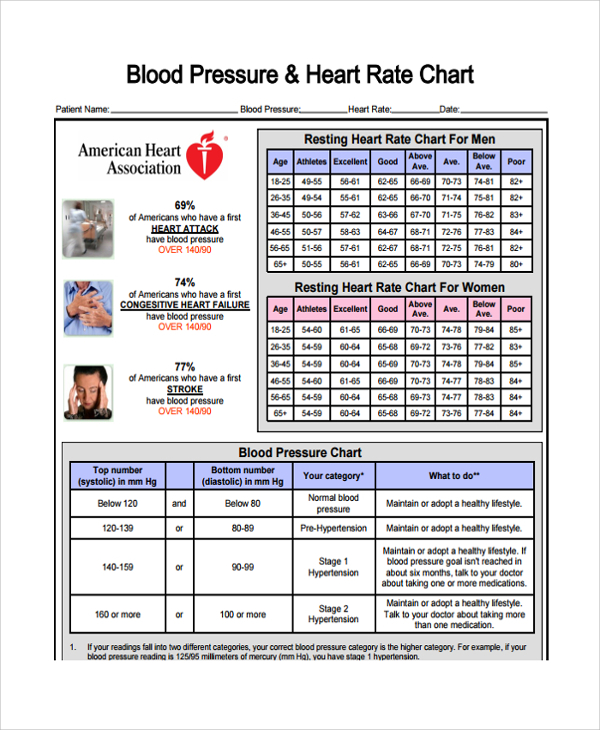 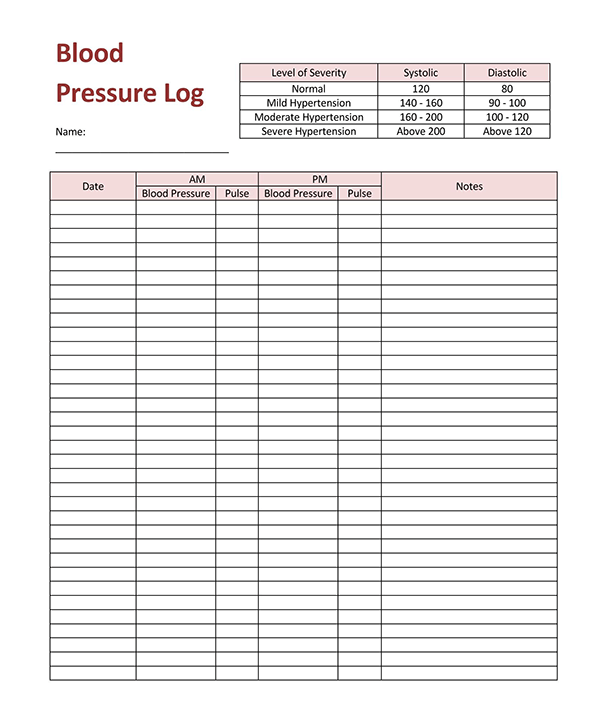
But drawing thresholds is a losing method when you have a continuous measure, like blood lactate. People would use one single blood test, like a blood lactate level, and then they would pick a threshold, above this or below that. And at that time, there was really nothing out there. So it was important at that time to not so much reinvent the diagnostic system, but to talk about how patients come in at different levels of severity. But people were relying on DRGs as a way to classify and identify patients, especially in the ICU. There’s little correlation to the clinical.  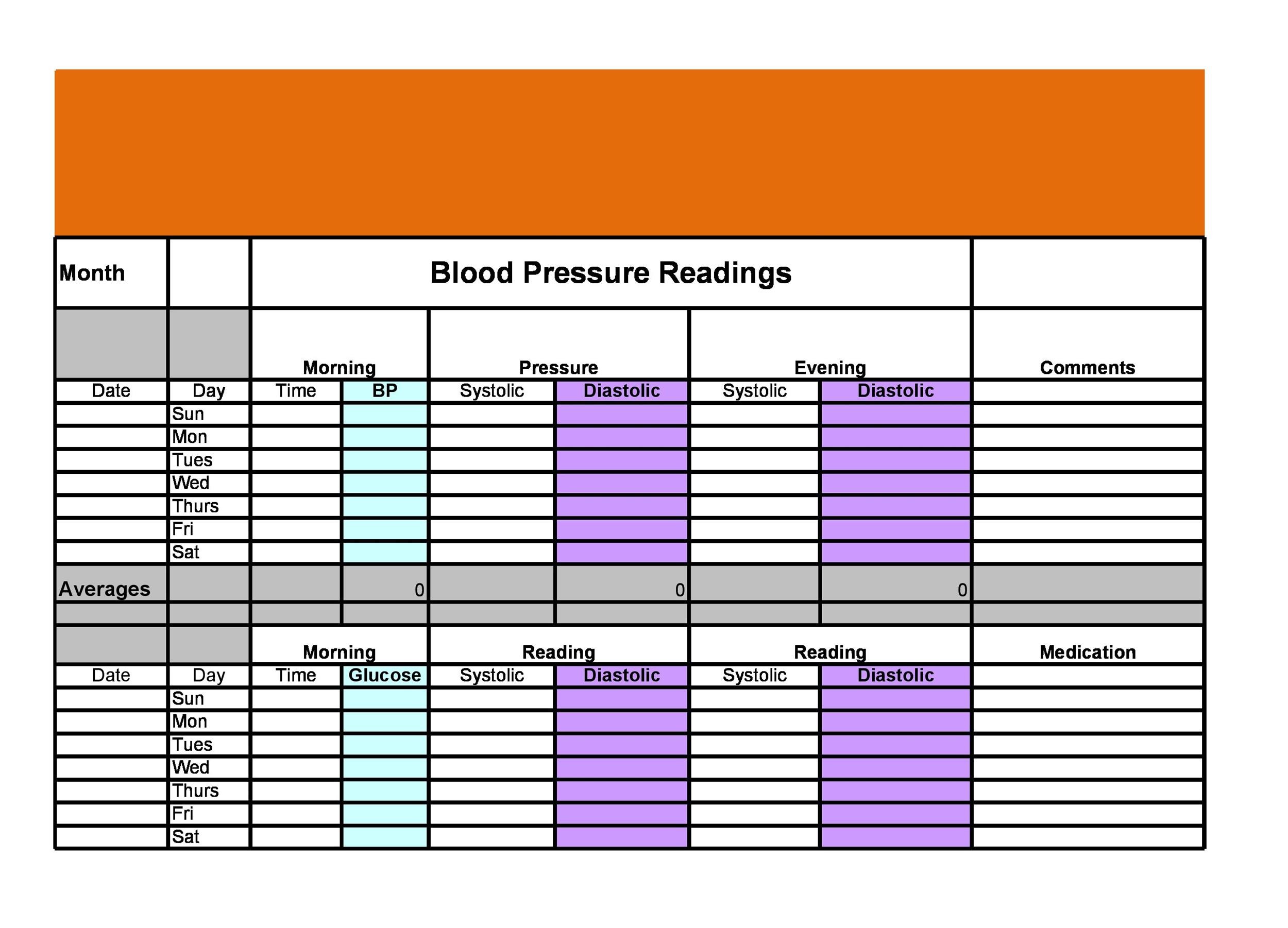
When we started in the 1970s, DRGs were just coming on the scene, and obviously they were oriented towards the business and financing aspects of healthcare. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
